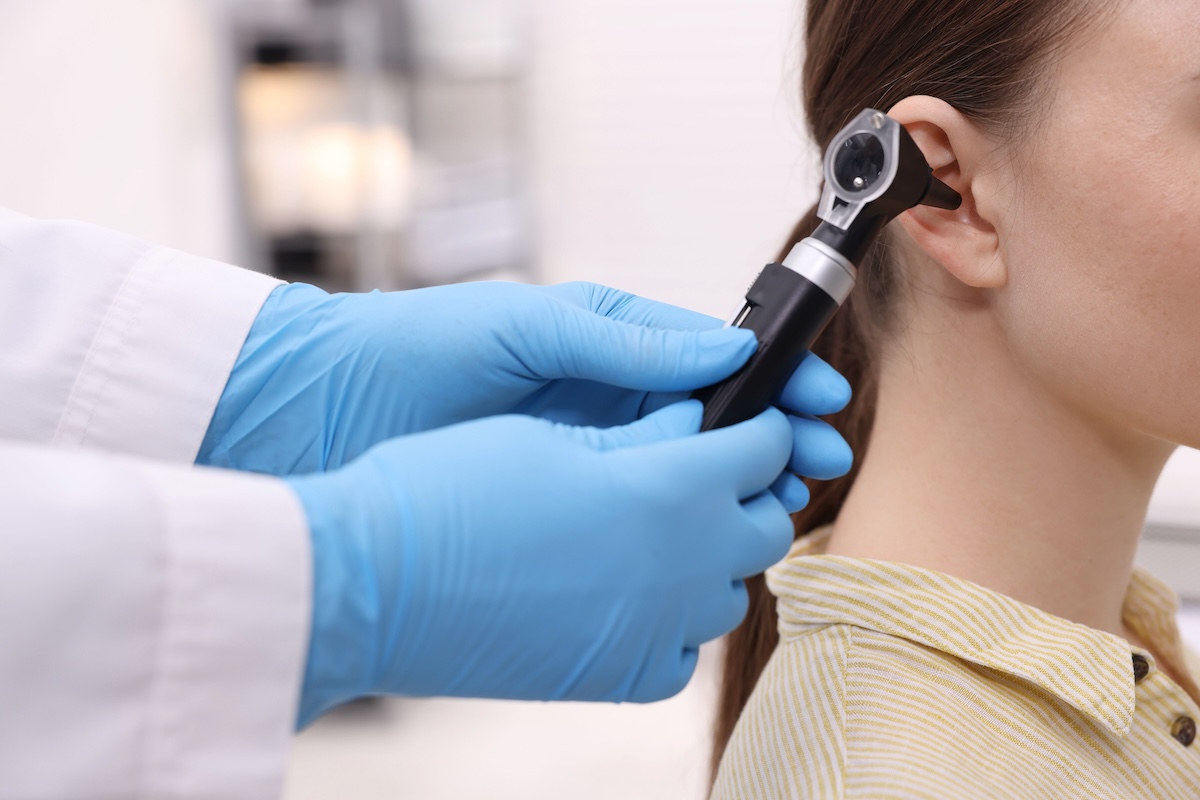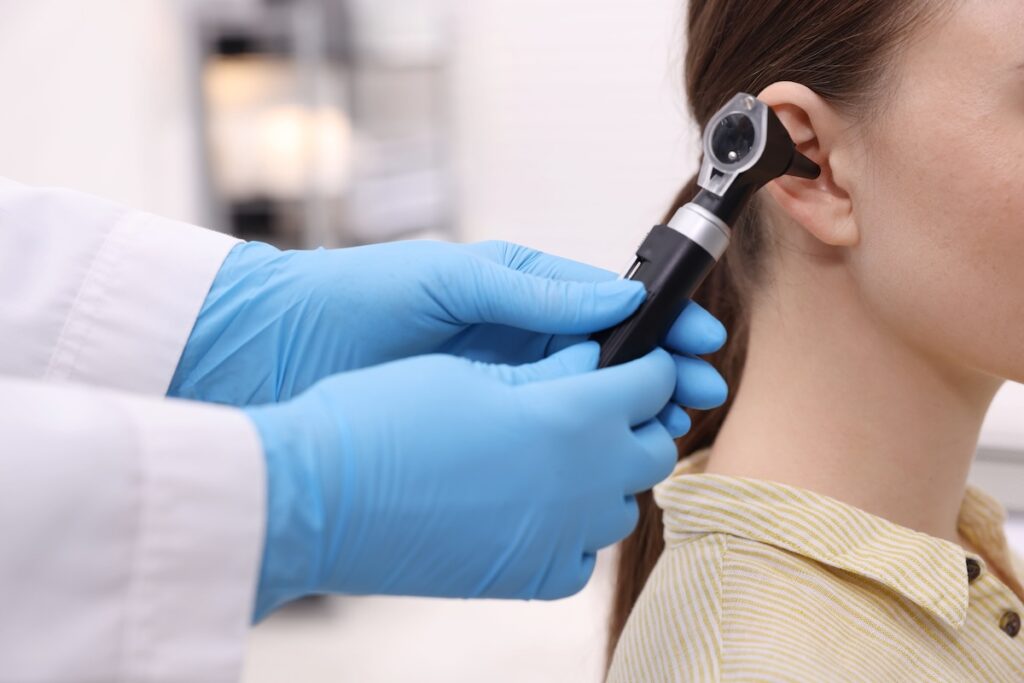
Hearing test. Doctor examining patient’s ear with otoscope in clinic, closeup
Practising optometrists are well aware of the effects of diabetes on the eye, but its impact on hearing often goes unnoticed. Dr. Mehwish Nisar, a research fellow at the Centre for Hearing Research at The University of Queensland, highlights the link between diabetes and hearing loss, providing practical guidance on screening and referral. By incorporating these strategies, optometrists can play a vital role in holistic care and improve outcomes for patients with diabetes.
The systemic and ocular changes that occur during the progression of diabetes mellitus are well-known to optometrists. However, the impact of diabetes on the auditory system is a less recognized but equally important consideration. Compelling evidence indicates that individuals with diabetes are twice as likely to experience hearing loss compared to those without the condition, with the risk increasing further with age and the duration of diabetes.
The Overlooked Link: Diabetes and Sensorineural Hearing Loss
The evidence base connecting diabetes and sensorineural hearing loss is robust and growing. Multiple epidemiological studies and meta-analyses demonstrate a higher prevalence and accelerated progression of sensorineural hearing loss in individuals with diabetes.
A recent analysis found significantly higher hearing loss rates in Type 2 diabetes patients versus controls (53% vs 25.2%, p < .0001), with 15% unilateral and 29.6% bilateral loss in the diabetic group (both p < .01).
Sensorineural hearing loss, the most common diabetes-associated hearing loss, involves inner ear or auditory nerve damage with insidious progression. The underlying pathophysiological mechanisms mirror those of diabetic retinopathy: microangiopathy impairs cochlear blood supply, neuropathy disrupts auditory nerve transmission, metabolic disturbances harm hair cells, and basement membrane thickening impedes exchange processes, all cumulatively affecting high-frequency hearing and speech comprehension.
Why Hearing Loss Matters in Comprehensive Diabetes Care
Untreated hearing loss profoundly impacts quality of life, causing social isolation, depression, and cognitive decline. Within diabetes management, hearing impairment disrupts essential patient-provider communication, compromising diabetes education, self-management, and treatment adherence, ultimately worsening health outcomes. Additionally, hearing loss independently increases fall risk, compounding existing diabetes-related concerns from peripheral neuropathy.
Early identification and intervention enable healthcare providers to mitigate these risks, enhancing overall patient wellbeing and optimizing comprehensive diabetes care outcomes.
Shared Pathophysiology: The Eye and the Ear
Both the retina and cochlea are highly specialized, metabolically active structures dependent on intricate microvascular networks, rendering them exceptionally vulnerable to diabetic injury. Emerging evidence strengthens this connection: studies demonstrate that individuals with proliferative diabetic retinopathy face significantly elevated hearing loss risk compared with those with non-proliferative or absent retinopathy.
This correlation positions advanced retinal disease as a systemic warning signal extending to auditory compromise.
Guidance for Optometrists: Integrating Hearing Awareness
Optometrists are ideally placed to identify at-risk patients for diabetes-related hearing loss. By incorporating simple screening strategies into routine clinical practice, they can facilitate timely referrals.
In-Practice Screening
The first step in identifying a potential hearing problem is to ask. A few targeted screening questions can be highly effective in flagging patients who may require further investigation. These questions should be asked of all patients with diabetes, regardless of age or retinopathy status. A positive response should prompt a recommendation for a formal hearing assessment.
Referral Triggers and Pathways
The decision to refer a patient for a hearing assessment should be based on a combination of the patient’s history, clinical findings, and risk factors. The presence of diabetic retinopathy, particularly PDR, should be considered a major red flag for other microvascular complications and should prompt a strong recommendation for a comprehensive hearing assessment.
If a patient expresses any concerns about their hearing, it is essential to document these in the patient’s record and to make a formal referral. The referral can be made to the patient’s general practitioner (GP), who can then coordinate a referral to an audiologist, or directly to an audiology clinic if local pathways permit.
Strengthening Interprofessional Referrals and Collaborative Care
Effective diabetes complication management demands collaborative, interprofessional approaches, with optometrists best positioned to initiate crucial hearing care referral pathways. Optimal care utilizes integrated electronic health records enabling seamless, secure information sharing among optometrists, GPs, endocrinologists, and audiologists, ensuring comprehensive patient profiles across providers.
Optometry practices should develop clear, formal referral protocols with local audiology clinics and GPs through pre-printed referral pads, digital templates, or secure messaging channels that streamline processes. Multidisciplinary team meetings and informal case discussions significantly enhance coordination for complex diabetic patients.
Detection and Preventive Opportunities
Early hearing loss detection in diabetic populations enables timely intervention, potentially slowing progression, improving communication, and enhancing quality of life. While standardised screening guidelines remain undeveloped, pragmatic approaches include baseline hearing assessment following diabetes diagnosis, periodic screenings every one to three years, particularly for patients with diabetic retinopathy, poor glycaemic control, or microvascular complications, and prompt assessment when hearing difficulties emerge.
Optometrists can employ opportunistic screening through simple questions to identify patients requiring formal audiological evaluation, a practical approach for busy practices. Formal audiological assessment by qualified audiologists using pure-tone and speech audiometry remains the diagnostic gold standard.
Population Considerations: Focus on At-Risk Groups
Specific population risks and cultural factors critically inform diabetes and hearing loss management. In Australia, Aboriginal and Torres Strait Islander peoples experience significantly elevated Type 2 diabetes rates with earlier onset and severe complications, alongside alarmingly high chronic otitis media rates and childhood-onset hearing loss, exacerbating diabetes-related hearing loss and creating profound auditory challenges.
Culturally and linguistically diverse immigrant communities also demonstrate higher diabetes prevalence and less utilization of hearing care services. Addressing these disparities requires accessible screening programs, culturally relevant educational materials, and robust partnerships with indigenous health services and multicultural community organizations for equitable, effective care delivery.
Looking Ahead: Integration in Diabetes Protocols
Future diabetes management requires integrated, patient-centered approaches transcending “siloed specialist care”. Protocols should incorporate routine holistic sensory screening using validated point-of-care tools, identifying both retinopathy and hearing loss in optometry and general practice settings. Enhanced interdisciplinary training would strengthen understanding and improve referral processes and collaborative management.
Technological innovations – tele-audiology and AI-powered remote screening – promise expanded accessibility in underserved populations, mirroring successful tele-ophthalmology models. Additionally, patient empowerment through comprehensive complication education will enhance self-management engagement and screening adherence, optimizing long-term visual and auditory health outcomes.
Hearing loss is a significant and often-overlooked complication of diabetes with a substantial impact on an individual’s quality of life. Optometrists, as primary eyecare providers, are in a unique position to identify patients at risk and facilitate early referral for auditory assessment. By recognizing the shared pathophysiology of the eye and the ear in diabetes, and by integrating simple screening questions and referral practices into their routine care, optometrists can play a vital role in improving the overall health and wellbeing of their patients with diabetes. The time has come to break the silence on diabetic hearing loss and embrace a more integrated approach to sensory care in diabetes management.