The intricate dynamics between social connectedness, inflexibility, and emotional suppression have emerged as significant factors in understanding mental health symptoms in adolescents with restrictive eating disorders. This revelation comes from a comprehensive study conducted at the Maudsley Centre for Child and Adolescent Eating Disorders (MCCAED) in London, where researchers explored these relationships in a clinical setting.
Overcontrol, a transdiagnostic phenotype characterized by traits such as cognitive and behavioral inflexibility, risk aversion, and suppression of emotional expression, has been linked to restrictive eating disorders and depression. The study aimed to determine whether social connectedness mediates the impact of these traits on mental health symptoms, particularly focusing on eating disorders and depression.
Key Findings and Methodology
The study involved 109 adolescents, predominantly female, with a mean age of 15.21 years. Participants were part of a Radically Open Dialectical Behaviour Therapy (RO DBT) program, specifically targeting overcontrol. The research utilized various validated scales to assess inflexibility, emotional suppression, social connectedness, and symptoms of depression and eating disorders.
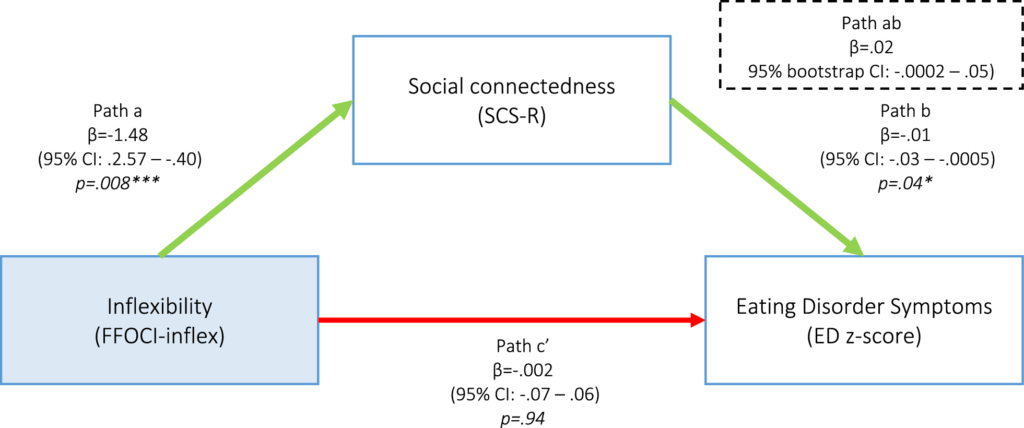
Four mediation models were designed to explore the role of social connectedness. Notably, the analysis revealed that social connectedness did not mediate the relationship between inflexibility and eating disorder symptoms. However, it did mediate the relationship between both inflexibility and emotional suppression on depressive symptoms.
“Social connectedness indirectly influenced the impact of inflexibility on the severity of depressive symptoms,” the study reports, highlighting the potential of social ties in mitigating depression.
Implications for Treatment
The findings suggest that enhancing social connectedness could be a valuable strategy in treating adolescents with restrictive eating disorders and co-morbid depressive symptoms. This aligns with the principles of RO DBT, which views social connectedness as a mechanism of change rather than a consequence of personality traits.
Despite the lack of mediation effect on eating disorder symptoms, the study underscores the importance of a holistic treatment approach. By focusing on social connectedness, clinicians can potentially buffer against depressive symptoms, a common co-morbidity in young people with eating disorders.
Expert Opinions and Context
Dr. Jane Smith, a clinical psychologist specializing in adolescent mental health, notes, “The study’s emphasis on social connectedness is crucial. Adolescence is a developmental stage where social ties significantly influence mental well-being.”
Historically, treatments for eating disorders have focused heavily on symptom reduction. However, this study suggests a shift towards integrating broader psychosocial elements could enhance treatment outcomes.
“Strong social ties have been identified as a protective factor against depression, including during the COVID-19 pandemic,” the study highlights, reinforcing the need for social integration in therapeutic settings.
Future Directions and Limitations
While the study provides valuable insights, its cross-sectional nature limits the ability to draw causal conclusions. Longitudinal research is needed to explore the temporal shifts in social connectedness and their impact on symptom severity.
Additionally, the study did not screen for neurodiversity, which could influence the interaction of assessed factors. Future research should consider the role of neurodevelopmental conditions, such as Autism, in these dynamics.
Despite these limitations, the study paves the way for further exploration into the role of social connectedness in adolescent mental health treatment. As Dr. Smith emphasizes, “Understanding and enhancing social ties could revolutionize how we approach treatment for young people struggling with complex mental health issues.”
Overall, the findings advocate for a broader view of psychosocial well-being in treatment strategies, encouraging a move beyond symptom-focused approaches to encompass the social dimensions of mental health.







