OAK BROOK, Ill. – A groundbreaking national study conducted in Denmark has revealed that a minimally invasive procedure known as ablation is as effective as traditional surgery for treating small kidney cancers. The study, which tracked nearly 1,900 patients over almost a decade, found that ablation offers faster recovery and fewer complications. These findings were published today in the journal Radiology, associated with the Radiological Society of North America (RSNA).
The research specifically targeted patients diagnosed with stage T1a renal cell carcinoma, a type of cancer increasingly discovered incidentally during CT scans for unrelated health issues, such as imaging of the prostate or ovaries. “These incidental cancers are putting increasing pressure on health care systems,” explained lead author Iben Lyskjær, Ph.D., M.Sc., associate professor at Aarhus University and Aarhus Hospital in Denmark. “While early detection improves outcomes, it also raises the need for better risk stratification and treatment options.”
Comparison of Ablation and Surgical Resection
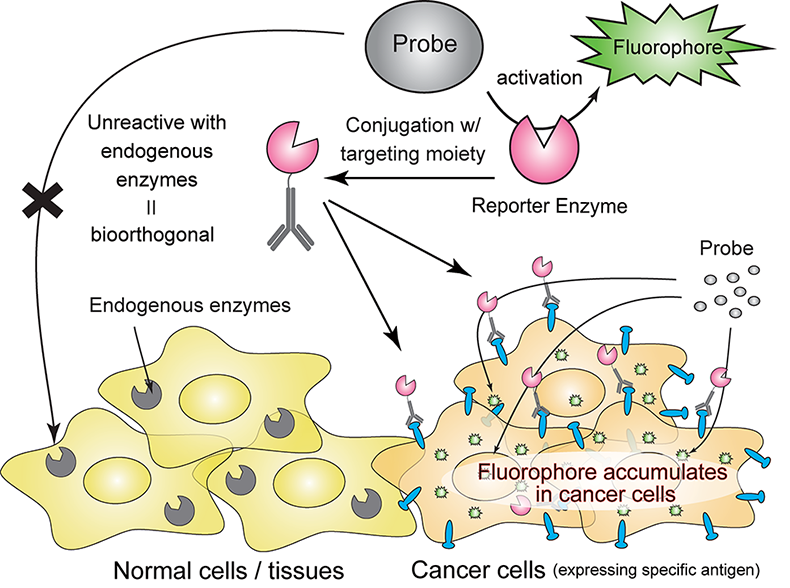
Surgical tumor resection has long been the standard treatment for stage T1a renal cell carcinoma. However, ablation has emerged as a promising alternative, potentially reducing complications, hospital stays, and costs. This image-guided procedure eradicates tumors using either extreme heat (radiofrequency ablation) or cold (cryoablation). Since its introduction in Denmark in 2006, ablation’s popularity has steadily grown.
Dr. Lyskjær and her team embarked on a nationwide registry-based cohort study of Danish adults diagnosed with T1a renal cell carcinoma between January 2013 and December 2021. Their objective was to compare outcomes between patients treated with ablation and those who underwent surgery. “This is not a single center but a nationwide study that reflects the everyday clinical practice in Denmark and what happens to real patients in a national health care system,” she noted.
Study Findings and Patient Outcomes
The study encompassed 1,862 patients, with a median age of 64, including 1,305 men. Participants were divided into three groups: the ablation group (540 patients), the resection group (1,002 patients), and the nephrectomy group (320 patients). Within the ablation group, 42 patients underwent radiofrequency ablation, while the remainder received cryoablation.
“There was no evidence of a difference in the risk of cancer progression between patients who had ablation and the resection group. However, local recurrence of the disease was more frequent following ablation than resection and nephrectomy (2.41%, 1.20%, and 0%, respectively).” – Dr. Iben Lyskjær
Despite the slightly higher local recurrence rate in the ablation group, Dr. Lyskjær emphasized that recurring tumors could be effectively treated with another ablation or surgery. Importantly, patients experiencing local recurrences did not exhibit worse overall survival rates.
Implications for Treatment Options
Distant metastasis, or the spread of cancer cells to distant organs or lymph nodes, was more common among patients who underwent nephrectomy (4.38%) compared to those who had resection and ablation (1.90% and 1.67%, respectively). Notably, ablation patients experienced the shortest hospital stays, with most returning home the same day. They also reported the fewest 30-day post-treatment hospital contacts, indicating fewer complications.
“Our study demonstrated that the overall progression rates were low across all treatment modalities, supporting the effectiveness of both ablation and resection for T1a renal cell carcinoma.” – Dr. Iben Lyskjær
Dr. Lyskjær highlighted the uncertainty surrounding whether incidentally discovered tumors would develop into aggressive cancers. “That’s a good reason to consider using a minimally invasive approach as a broader treatment option,” she stated. “The best choice depends not only on the patient’s characteristics but also on the patient’s preferences. We should be showing patients data and asking the patients what kind of treatment they want.”
Looking Forward: Broader Implications
This study’s results could significantly influence treatment strategies for small kidney cancers, offering patients more options and potentially easing the burden on healthcare systems. As the medical community continues to explore minimally invasive procedures, ablation could become a standard recommendation for suitable candidates, balancing efficacy with patient comfort and recovery.
As researchers and healthcare providers digest these findings, the focus will likely shift towards refining patient selection criteria and optimizing treatment protocols to ensure the best possible outcomes for those diagnosed with stage T1a renal cell carcinoma.