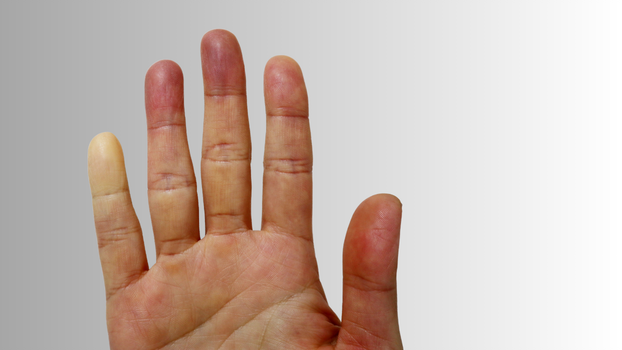
Researchers at The Institute have discovered that botulinum toxin, commonly known as Botox, is a promising treatment for severe finger lesions associated with autoimmune diseases such as systemic sclerosis. This revelation, published in JAMA Dermatology, suggests that Botox injections could effectively manage debilitating conditions caused by reduced blood flow to the fingers, including acute digital ischemia, digital ulcers, and gangrene.
The study, a systematic review and individual-patient data meta-analysis, examined 30 published studies and one unpublished case involving 119 patients. It found that Botox treatment, which works by reducing blood vessel constriction and improving circulation, led to the complete healing of lesions in more than 85% of patients. These conditions, often resistant to standard therapies, can cause severe pain, infections, and tissue destruction, sometimes resulting in amputation.
Understanding Systemic Sclerosis and Its Challenges
Systemic sclerosis, a rare and chronic autoimmune disease, is characterized by excessive tissue hardening and narrowing of small blood vessels, affecting both the skin and internal organs. It is the most common cause of the severe finger lesions studied. Other related conditions include lupus and rheumatoid arthritis, which also impact blood vessels and the immune system.
“These new findings are particularly important because therapeutic options remain limited for the cutaneous and vascular manifestations of systemic sclerosis and other autoimmune diseases,” says Dr. Elena Netchiporouk, a senior author of the study and a scientist at the Research Institute of the McGill University Health Centre (MUHC). “Current vasodilator and immunosuppressive treatments are often costly, minimally effective, and associated with significant adverse effects.”
Expertise and Innovation at MUHC
Dr. Netchiporouk, a dermatologist specializing in autoimmune diseases at MUHC, has been using Botox injections in her clinical practice for four years to treat severe Raynaud’s phenomenon, acute digital ischemia, ischemic ulcers, and early-stage gangrene. One notable case involved a patient in his fifties suffering from digital necrosis due to a rare autoimmune disease. Conventional treatments failed, but Botox injections provided significant relief.
“The injections relieved the pain and improved sensation within 24 hours, and the necrosis improved after two weeks,” Dr. Netchiporouk explains. “This treatment has become an important tool, especially for patients with autoimmune vascular diseases that result in serious health consequences and for which there are few therapeutic options.”
An Effective and Safe Outpatient Treatment
The simplicity and speed of Botox administration make it an advantageous option for outpatient settings. The studies reviewed reported few adverse effects, which were generally mild and short-lived, such as temporary muscle weakness or pain at the injection site.
“Our results show that botulinum toxin can be used to improve blood circulation in the fingers and treat serious complications such as ulcers or gangrene,” says Dr. Catherine Zhu, a dermatology resident at MUHC and first author of the study. “This offers a safe and easy-to-administer alternative, potentially reducing reliance on intravenous therapies that require hospitalization and lowering healthcare costs.”
Beyond Raynaud’s Phenomenon
Raynaud’s phenomenon, marked by spasms that impair blood circulation in the fingers and toes, is common in systemic sclerosis and other autoimmune diseases. It can lead to serious complications such as ulcers, gangrene, or even amputation. While previous studies have explored Botox’s effectiveness for Raynaud’s, this new study is the first to focus exclusively on advanced ischemic complications.
Among the 119 cases reported, systemic sclerosis was the cause in 61% of cases, other systemic autoimmune diseases in 12%, and trauma in 9%. The rest were due to peripheral arterial diseases or drug-induced vessel constriction.
The study’s findings suggest that Botox is particularly effective for skin complications caused by systemic sclerosis and other autoimmune diseases. In most cases, a single injection session was sufficient to achieve the desired response.
“Our conclusions support my clinical observations and those of several other colleagues: botulinum toxin can offer significant benefits with a favorable safety profile,” Dr. Netchiporouk emphasizes. “It deserves further study to develop standardized protocols and optimize outcomes.”
Looking Ahead
The study, “Botulinum Toxin for Refractory Digital Ischemia and Ulcers in Systemic Sclerosis- A Systematic Review and Meta-Analysis,” authored by Catherine Zhu and colleagues, represents a significant step forward in treating autoimmune-related vascular complications. As researchers continue to explore Botox’s potential, it may become a cornerstone treatment for conditions previously considered difficult to manage.
With the promise of improved patient outcomes and reduced healthcare costs, the medical community eagerly anticipates further research and potential protocol development for this innovative treatment approach.







