More than 10,000 Americans suffering from chronic liver disease are currently on a waitlist for a liver transplant, a life-saving procedure that remains out of reach for many due to a shortage of donated organs. Furthermore, some patients with liver failure are deemed ineligible for transplants because their health cannot withstand the rigors of surgery.
In a groundbreaking development, engineers at the Massachusetts Institute of Technology (MIT) have unveiled a potential solution: injectable “mini livers” designed to take over the functions of a failing liver. In a recent study conducted on mice, these injected liver cells demonstrated viability in the body for at least two months, producing vital enzymes and proteins typically generated by the liver.
Revolutionary “Satellite Livers”
Professor Sangeeta Bhatia, a leading researcher in health sciences and technology at MIT, describes these innovations as “satellite livers.” She explains, “If we could deliver these cells into the body, while leaving the sick organ in place, that would provide booster function.” Bhatia, who is also affiliated with MIT’s Koch Institute for Integrative Cancer Research and the Institute for Medical Engineering and Science (IMES), is the senior author of this pioneering study published in the journal Cell Biomaterials.
MIT postdoctoral researcher Vardhman Kumar, the lead author of the study, and his team have been exploring methods to restore liver function without the need for invasive surgery. The human liver is responsible for around 500 essential tasks, including blood clot regulation, bacteria removal from the bloodstream, and drug metabolism. These functions are primarily performed by hepatocytes, the liver’s main cell type.
Engineering a New Approach
Over the past decade, Bhatia’s lab has focused on strategies to restore hepatocyte function. One potential method involves embedding hepatocytes into a biomaterial like a hydrogel, but this requires surgical implantation. To bypass surgery, the team explored injecting hepatocytes directly into the body. They enhanced this approach by developing an engineered niche to improve cell survival and enable noninvasive monitoring of graft health.
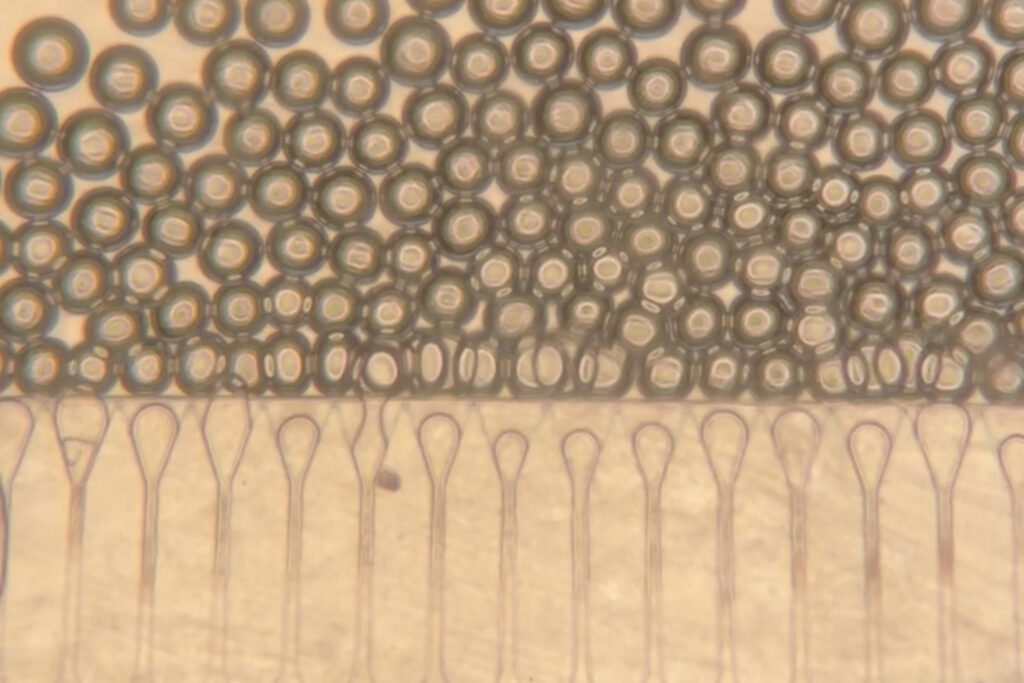
The researchers innovatively combined hepatocytes with hydrogel microspheres, which help the cells maintain cohesion and connect with nearby blood vessels. These microspheres possess unique properties, allowing them to behave like a liquid when closely packed, facilitating injection through a syringe. Once inside the body, they regain a solid structure, supporting the formation of stable tissue grafts.
“What we did is use this technology to create an engineered niche for cell transplantation,” Kumar explains. “If the cells are injected in the absence of these spheres, they would not integrate efficiently with the host.”
Potential for Widespread Application
In collaboration with Nicole Henning, an ultrasound research specialist at the Koch Institute, the team developed a technique to inject the cell mixture using ultrasound-guided syringes. This method also allows for the long-term monitoring of the implant’s stability. In the study, mini livers were injected into the fat tissue in the belly, but future applications could see them delivered to other body sites, such as the spleen or near the kidneys.
As Kumar notes, “For a vast majority of liver disorders, the graft does not need to sit close to the liver.” This flexibility could expand the treatment’s applicability across various conditions.
Testing and Future Prospects
In mouse tests, the researchers injected the liver cell and microsphere mixture into perigonadal adipose tissue, a type of fatty tissue. The cells formed a stable, compact structure, with blood vessels growing into the graft area over time. This vascularization is crucial for the hepatocytes’ survival and function.
“The new blood vessels formed right next to the hepatocytes, which is why they were able to survive,” Kumar says. “They were able to get the nutrients delivered right to them, they were able to function the way they’re supposed to.”
The cells remained viable and active for eight weeks, suggesting potential for long-term treatment of liver disease. This technology could serve as an alternative to surgery or as a bridge to transplantation, providing support until a donor organ becomes available.
Challenges and Future Directions
While promising, the current technology requires patients to take immunosuppressive drugs. Researchers are exploring the development of “stealthy” hepatocytes that could evade the immune system or using hydrogel microspheres to deliver immunosuppressants locally.
This research, supported by the Koch Institute Support grant from the National Cancer Institute, the National Institutes of Health, the Wellcome Leap HOPE Program, a National Science Foundation Graduate Research Fellowship, and the Howard Hughes Medical Institute, represents a significant step forward in addressing the challenges of liver disease treatment.
As the field of regenerative medicine continues to advance, these injectable mini livers could transform the landscape of liver disease treatment, offering new hope to thousands of patients awaiting transplants.






