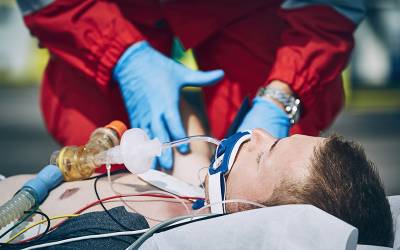
Researchers have uncovered compelling evidence that prehospital emergency intubation of high-risk trauma patients could significantly improve survival rates. A study published in The Lancet Respiratory Medicine suggests a 10.3% increase in 30-day survival rates, potentially saving 170 lives annually in the UK.
This groundbreaking analysis, supported by artificial intelligence (AI), provides the strongest evidence yet that prehospital emergency anesthesia with intubation is crucial for those most in need. Trauma remains the leading cause of death among children and adults under 40 in England and Wales, yet there has been a lack of high-quality evidence regarding the optimal timing for certain critical interventions, such as the insertion of breathing tubes.
The Role of AI in Trauma Care
The study utilized AI-assisted modeling to predict which patients would benefit most from intubation and to isolate the impact of the procedure from other factors like injury severity. Researchers developed a machine learning model, ‘Intub-8’, which used eight prehospital measurements to predict outcomes.
Among the 229 high-risk patients identified by the model as needing intubation, those who received it before hospital arrival were 10.3% more likely to survive within a 30-day period compared to those who did not. Scaling these findings to a national level suggests that implementing prehospital intubation for all eligible trauma patients could save 170 lives annually.
“The airway is a top priority in major trauma, but the question of whether we should intubate before hospital arrival is unsettled because we cannot ethically conduct a randomized trial,” said Dr. Amy Nelson, joint first author from UCL Queen Square Institute of Neurology and King’s College London.
Implications for Healthcare Policy
The findings could significantly influence policy discussions on funding specialist prehospital critical care teams. Currently, in the UK, prehospital intubation is primarily provided by air ambulance services, which are specially trained and equipped for such interventions. The study suggests that expanding these services or training ground ambulance teams could enhance trauma care.
According to the researchers, the cost-effectiveness analysis indicates potential savings of £101 million annually for the UK, due to reduced costs of further care and lives saved. This financial aspect could further support arguments for increased funding and resources for prehospital critical care.
“In medicine, action and inaction are not morally asymmetric. When we cannot have randomized controlled trial evidence for an intervention, we must use the best available alternative: causal inference from real-world data, assisted by artificial intelligence,” stated Professor Parashkev Nachev, joint senior author.
Global and Local Context
Associate Professor Julian Thompson, another joint senior author, emphasized the global impact of these findings. Advanced air ambulance services worldwide have struggled to assess the benefits and cost-effectiveness of their interventions. The use of AI in this study provides a new perspective on the significant impact of advanced care delivered before hospital arrival.
However, the authors caution that the findings are specific to the UK’s mixed rural-urban setting, where physician-paramedic teams perform all prehospital intubation. The survival benefits may vary in different healthcare systems or national contexts, underscoring the need for further research to explore long-term outcomes and potential complications.
“Using machine learning to model the effects of anesthesia delivered at the scene of accidents, the authors of this study have provided high-quality evidence that consistent provision of this intervention by pre-hospital teams not only saves many lives but does it in a cost-effective manner,” commented Professor David Lockey, Immediate Past Chair, Faculty of Pre-hospital Care, Royal College of Surgeons of Edinburgh.
The study, funded by Wellcome and the National Institute for Health and Care Research UCLH Biomedical Research Centre, represents a significant step forward in trauma care. It highlights the potential for AI to transform medical decision-making and improve patient outcomes, paving the way for more informed policy decisions and resource allocation in emergency healthcare.






